INTRODUCTION
[18F]Fluoro-2-deoxy-D-glucose positron emission tomography-computed tomographic (FDG-PET/CT) imaging constitutes an irreplaceable guiding tool in the diagnosis, staging, and management of non-small-cell lung carcinoma (NSCLC) due to its high sensitivity 0.81 (95% CI: 0.63–0.92) and specificity 0.96 (95% CI: 0.94–0.98)1,2. Nevertheless, false positives due to increased FDG uptake in physiological areas such as salivary glands, thyroid, thymus, among others, inflammatory processes, and foreign body reactions transpire, and we should remain vigilant to avoid unnecessary interventions. We present this patient case to highlight the significance of this phenomenon and indicate the need for further investigations regarding the use of FDG-PET/CT in the follow-up of an asymptomatic patient after a curative-intent surgical procedure.
CASE PRESENTATION
A 54-year-old, Caucasian, 160 cm, 55 kg, female patient with controlled hypertension presented in our department with a positive FDG-PET/CT while being in active surveillance for 13 years after a middle lobectomy. Written informed consent was obtained from the individual to publish any potentially identifiable images or data in this article. She was first diagnosed with two synchronous lesions in 2007, a clear cell renal cell carcinoma and a pulmonary nodule in the middle lobe. After a joint consultation with her oncologist, a plan of action was formulated, which comprised two sequential surgeries with curative intent. First, she underwent a right nephrectomy in February of 2007 and a month later the middle lobectomy was performed. Histopathology revealed that the pulmonary nodule was a metastatic lesion. Subsequently, the patient reached complete remission and was referred to follow-up with CT scans. In March 2020, and while the patient was asymptomatic and in active surveillance, a solid pulmonary nodule was detected in a scheduled follow-up CT. A multidisciplinary board constructed a differential diagnosis of local recurrence, a new cancer, and lipoid pneumonia, among others, which led to further testing in order to establish a diagnosis and define the appropriate course of management. For the reasons above, an FDG-PET/CT was performed, indicating potential findings for local recurrences in the bronchial stump with an SUVmax of 5.9 (Figure 1). Therefore, an EBUS bronchoscopy with FNA was performed to establish a diagnosis, nonetheless it came back negative. The blood assessment was also negative for an inflammatory process.
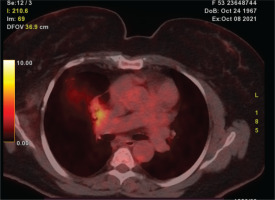
Figure 1
[18F]FDG-PET/CT scan showing a positive pulmonary nodule adjacent to the bronchial stump (SUVmax: 5.9)
Thereupon and after a joint oncological consultation, which considered the use of other diagnostic tools to establish diagnosis, such as navigational bronchoscopy, EUS, CT with needle biopsy, and surgery, we opted for a surgical approach, and a redo right thoracotomy was performed in May 2020. Intra-operatively, we encountered strong adhesions to the mediastinum, and a solid composition lesion that strongly adhered to the bronchial stump, fissure, and right hilum, was identified. Macroscopically the lesion had a caramel color and resembled a foreign body, the lesion was excised, and biopsies were taken from the lymph node stations 10/11 R as well. The patient had an uncomplicated recovery; the chest drain was removed on the fourth day of the post-operation, and she was discharged from the hospital the next day. Afterwards, she was referred to follow up with CT imaging, which was uneventful. The histological review revealed that the solid components consisted of calcifications and chronic inflammatory cells with multinucleated giant cells constituting a foreign body (Figure 2). The lymph nodes were negative for malignancy. The final report confirmed the use of bioglue at the bronchial stump.
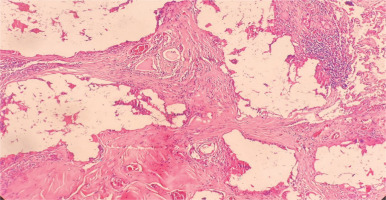
Figure 2
Hematoxylin and eosin stain (100×). Fibrous tissue with foreign-body type giant cell granulomatous reaction around clear spaces containing foreign material
Patient perspective
Following the surgical treatment that she underwent, the patient felt well, without any complaints. The patient had expressed that she was satisfied with the recommended treatment and expressed relief that the histopathological review showed no cancer. The patient continued her follow-up and her prognosis remains favorable. The patient reported no alterations in their quality of life during the evaluation.
DISCUSSION
[18F]Fluoro-2-deoxy-D-glucose PET/CT imaging is a well-established non-invasive tool that is used for the diagnosis, restaging and monitoring of lung cancers. There are inherent challenges in interpreting FDG-PET/CT imaging in the post-operative patient. Its specificity is limited because of the elevated FDG concentrations caused by post-operative inflammation. To prevent misinterpretations, it is recommended that the FDG-PET/CT is performed 1–2 months after surgery to avoid over staging. Careful examination of the CT component is vital because it can provide valuable additional information (abscess, granulomas). These conditions are often visible in the intravenous contrast media injection CT scan.
Persistent air-leakages after pulmonary resection are a common complication. They are generally of parenchymal (alveolar) etiology or caused by the staplers in an emphysematous parenchyma.
In an attempt to control air leakages after major pulmonary resections, surgical adhesives such as BioGlue® (Cryolife, Inc., Kennesaw, GA, USA) are used, which is a bio-adhesive comprising glutaraldehyde and purified bovine serum albumin, producing a stable, solid medium after these two components intertwine. Following the use of BioGlue® to a surgical area, an inflammatory response of macrophages, neutrophils, granulation tissue, and eventually a fibrous scar develops, consequently3,4. A foreign body reaction to the bio-adhesive can burgeon following two pathways: the aseptic fibrous or the exudative type. After 24-h, an exudative inflammation is presented, and at days 8 to 13, granulomatous inflammation takes place constituting a chronic inflammation. [18F]Fluoro-2-deoxy-D-glucose using the cells glucose transporter proteins located in the cell membrane enters the cell and undergoes phosphorylation by hexokinase enzyme and follows the glycolysis pathway, but unlike glycose [18F]Fluoro-2-deoxy-D-glucose cannot undergo phosphorylation leading to its increased accumulation and entrapment in cancer and inflammatory cells compared to normal tissue. The molecular factors guiding this phenomenon include: a low glucose-6-phosphatase enzyme activity, an over-expression of glucose transport membrane proteins, and an increased hexokinase enzyme activity. In vitro studies revealed an increased [18F] Fluoro-2-deoxy-D-glucose uptake in granulomas and inflammatory cells due to markedly elevated glycolysis in macrophages, neutrophils, and lymphocytes as described by the aforementioned pathways. Consequently, due to a foreign body reaction to the bio-adhesive, granulomas can potentially display false-positive PET images5-7.
In an attempt to attenuate the ability of the PET scan to differentiate between malignant and inflammatory tissue and consequently reduce the false positives regarding cancer diagnosis, the dual-time-point imaging (DTPI) and delayed-time-point imaging techniques were examined as a promising solution. In DTPI and delayed-time-point imaging, the PET scan was performed at a standard time point and repeated after a certain amount of time, leading to the conclusion that the SUV, which was obtained by the delayed image, has greater specificity in detecting and differentiating malignant from benign or inflammatory lesions8. The rationale was based on the assumption that the inflammatory cells progressively display a [18F]Fluoro-2-deoxy-D-glucose washout. The results of this procedure did not prove reliable in differentiating malignant from benign causes.
The CT images with IV contrast media injection deliver valuable information for the aforementioned question, in addition to the operative reports. These should include the implementation of surgical materials and sites where they were employed3.
Strengths and limitations
The strengths of this case report stem from the in-depth narrative study and management of this patient, which will serve as an educational tool and highlight our ability to generate hypotheses regarding the management of similar patients in the future. The main limitation stems from the nature of a case report, which cannot deliver quantitative data or prove cause-effect relationship, nor allow generalizations.
CONCLUSION
We should remain cognizant of pathological findings on follow-up [18F]Fluoro-2-deoxy-D-glucose-PET/CT for local recurrence adjacent to the resected zone in an asymptomatic patient with resected NSCLC, to avoid unnecessary biopsies and surgical procedures. Furthermore, using bioglue at the bronchial stamp as a sealant remains a topic for active research and a high degree of clinical and radiological precision for differential diagnosis is warranted. Lastly, it will significantly benefit the patient and the thoracic surgery community as a whole, the evolution of the PET CT as a diagnostic tool to differentiate between malignant and inflammatory tissue, and consequently reduce the false positives regarding cancer diagnosis or recurrences.



